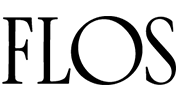Diverticulitis can be described as a digestive disorder and it affects the colon particularly. This is a prevalent problem, although it primarily affects elderly people; however, it is still not well known enough. This blog focuses on giving the reader, an extensive knowledge on diverticulitis in terms of the causes, signs, diagnosis, management, and how to prevent it. At the end of it, you should be able to have some clarity concerning this condition and how best to deal with it.
What is Diverticulitis?
Diverticulitis is usually diagnosed when small, weaker pockets which are referred to as diverticula swell up or, worse, get infected. These pouches which are most likely to be found in the low part of the large intestine known as the colon, arise from facets of the intestinal walls. Diverticula or also called diverticulosis is fairly benign and is generally asymptomatic, but diverticulitis can be a real pain and lead to complications.
The exact causes of diverticulitis are yet unknown, and however, it is considered to be caused by, among others, a diet low in fiber, the aging process, and physical inactivity. When diverticula start to fill up with waste material, it is probable that bacteria may swarm in and cause inflammation or infection. A diverticular disease is indicated by inflammation or infection of a diverticulum; this would involve; Abdominal pain typically localized to the left lower quadrant, condition associated with fever, nausea and vomiting, bloating and changes in bowel habits such as constipation or diarrhea.
The common diagnostic procedures include a physical examination, blood tests, and, a CT scan to help determine whether there is inflammation or any complication. For this type of condition, the patient may be advised to take liquids only, be prescribed antibiotics for infection and required to take analgesic drugs that can easily be bought from the counter. In some instances, the condition warrants admission to the hospital, administration of intravenous antibiotics, or even surgical intervention if processes such as abscesses, perforations, blockage occur.
The prevention of diverticulitis is fundamental by mainly avoiding the inclusion of a low-fiber diet, less fluid intake, and lack of physical activity. Much can be done for the prevention of diverticulitis in cases of diverticulosis with a proper management and certain change in the daily regimen of the patient.
Diverticulosis vs. Diverticulitis
Diverticulosis:
In diverticulosis, smaller sac-like protrusions referred to as diverticula develop in the walls of the digestive pipe commonly in the colon. These pouches are formed as a result of pressure build up within the colon and that leads to formation of hernias on the weak areas in the intestinal lining. Diverticulosis is commonly seen in older people, because as the colon ages it undergoes a process of elastic decline.
In fact, most of the patients with diverticular disease have no symptoms and are diagnosed by chance in sigmoidoscopy, colonoscopy or barium enema. Nevertheless, certain people may experience symptoms such as gurgling stomach, gas, and alterations of the bowel movements. The main causes of diverticulosis have not been fully determined, but various several believe that they may result from the low fiber diet, inactivity and hereditary factors.
The main treatment of diverticulosis is therefore conservative and mainly focused on nutrition and life style changes. The problem with constipation, therefore, can be alleviated by the assimilation of more fiber in fruits, vegetables, and whole grains as they lessen the pressure put on the colon by softening the stool. It also helps to maintain a good digestion system that comes with the intake of many water and exercises. Nevertheless, diverticulosis is a condition that rarely produces symptoms in its primary stage, but if a certain diverticulum becomes inflammation or infected it can result in diverticulitis. Diverticulosis can nevertheless be controlled with proper checkups, good health and living free of stress, among other things.
Diverticulitis:
Diverticulitis can be described as a state in which the pouches that exist in the large intestines known as diverticula get to swell or in other instances get infected. These pouches are commonly found in the colon and they develop because of the formation of defects in the lining of the intestines. Hence, though most people with diverticula or what is referred to as diverticulosis are asymptomatic, that is, they have no or minimal disturbing symptoms, diverticulitis is a different ball game; it can indeed be a real painful condition that may cause not just discomfort but major medical complications.
At present the manufacturers have not determined the root cause of diverticulitis but consider the consumption of low fiber diet, with advancing age and lack of exercises as causing factors. The waste that is not expelled from the intestines may accumulate in the pouches called diverticula and due to this, bacteria begin to grow and can cause inflammation or infection. Diverticulitis’s manifestations include sharp pain in the left inferior quadrant or the whole abdomen, increased temperature, nausea, vomiting, bloating, and changes in bowel habits or constipation.
A physical examination, complete blood count, and CT scan are some of the tests administered to diagnose diverticulitis and rule out inflammation or complications. The mild cases require the patients to be put on a liquid diet, antibiotics, and pain controlling agents, while they rest. In serious instances they may need to be hospitalized and may require intravenous antibiotics or surgery if there are complications, for example if the appendix has become gangrenous, ruptured, or created abscesses or bowel obstructions.
Strategies used in the prevention of diverticulitis include; taking high fiber diet, adequate intake of fluids and engaging in regular physical exercises. Based on these lifestyle changes, people with diverticulosis will live normal, symptomless lives with a low risk of developing diverticulitis.
Causes of Diverticulitis
The exact cause of diverticulitis is not entirely understood, but several factors are believed to contribute to its development:
Diet:
A low-fiber diet is considered a significant risk factor. Fiber helps keep stools soft and reduces pressure on the colon. A lack of fiber leads to harder stools, which can increase pressure within the colon and contribute to the formation of diverticula.
Aging:
As people get older, the walls of the colon can become weaker, making it easier for diverticula to form.
Genetics:
There is some evidence to suggest that a family history of diverticulitis may increase your risk.
Obesity:
Being overweight is associated with a higher risk of diverticulitis.
Lack of Exercise:
Regular physical activity helps maintain healthy bowel function, and a sedentary lifestyle can contribute to the development of diverticulitis.
Smoking:
Smokers may have an increased risk of developing diverticulitis compared to non-smokers.
Symptoms of Diverticulitis
Diverticulitis Points
Abdominal Pain:
Often the most common symptom, typically felt in the lower left side of the abdomen. The pain may be sudden and severe, or it can start out mild and worsen over several days.
Fever:
An elevated body temperature is common, indicating an infection.
Nausea and Vomiting:
These symptoms often accompany abdominal pain and fever.
Changes in Bowel Habits:
These may include constipation, diarrhea, or a frequent need to urinate.
Bloating and Gas:
General feelings of abdominal discomfort.
Loss of Appetite:
A decrease in desire to eat due to discomfort and other symptoms.
In severe cases, complications such as abscesses, fistulas, or blockages in the colon can occur, which require immediate medical attention.
Diagnosing Diverticulitis
If you experience symptoms of diverticulitis, it’s important to seek medical advice. Diagnosis typically involves several steps:
Medical History and Physical Exam:
Your doctor will review your medical history and perform a physical examination, focusing on the abdomen to check for tenderness.
Blood Tests:
These can help identify signs of infection, such as an elevated white blood cell count.
Imaging Tests:
A CT scan is the most common imaging test used to diagnose diverticulitis. It can reveal inflamed or infected pouches in the colon and help determine the severity of the condition.
Colonoscopy:
While not typically used to diagnose an acute attack of diverticulitis, a colonoscopy might be performed after treatment to rule out other conditions and assess the extent of diverticulosis.
Treatment Options for Diverticulitis
The treatment for diverticulitis depends on the severity of the symptoms and whether complications are present.
Mild Diverticulitis
For mild cases, treatment typically involves:
Antibiotics:
These are prescribed to treat the infection. Common antibiotics include metronidazole combined with ciprofloxacin or amoxicillin-clavulanate.
Dietary Changes:
A clear liquid diet may be recommended initially to allow the colon to heal. As symptoms improve, a gradual return to a regular diet is advised, starting with low-fiber foods and gradually increasing fiber intake.
Pain Relievers:
Over-the-counter pain medications like acetaminophen can help manage discomfort. Nonsteroidal anti-inflammatory drugs (NSAIDs) are generally avoided as they can increase the risk of complications.
Severe Diverticulitis
Severe or complicated diverticulitis may require more intensive treatment, including:
Hospitalization:
This may be necessary for intravenous antibiotics and fluids if oral antibiotics are insufficient.
Surgery:
If there are complications such as abscesses, perforations, or significant blockages, surgery may be required to remove the affected part of the colon. Types of surgery include:
Primary Bowel Resection:
The diseased part of the intestine is removed, and the healthy sections are reconnected. This can often be done through minimally invasive (laparoscopic) surgery.
Bowel Resection with Colostomy:
If there is too much inflammation to reconnect the colon, a temporary colostomy may be performed. This involves creating an opening (stoma) in the abdominal wall to divert waste into a colostomy bag. The colostomy is usually reversed once the inflammation has healed.
Preventing Diverticulitis
While it’s not always possible to prevent diverticulitis, several lifestyle changes can help reduce your risk:
High-Fiber Diet:
Consuming a diet rich in fiber can help prevent constipation and reduce pressure on the colon.
Hydration:
Drinking plenty of fluids helps keep stools soft and easier to pass.
Regular Exercise:
Regular physical activity supports healthy bowel function and helps prevent constipation.
Healthy Weight:
Maintaining a healthy weight through diet and exercise can lower your risk of developing diverticulitis.
Avoid Smoking:
Quitting smoking can reduce your risk of diverticulitis and other health issues.
Respond to Bowel Urges:
Don’t delay bowel movements, as holding in stools can increase pressure on the colon.
Living with Diverticulitis
For those diagnosed with diverticulitis and ed are same, managing the condition involves a combination of medical treatment and lifestyle adjustments. Here are some tips for living with diverticulitis:
Follow Medical Advice:
Adhere to your doctor’s recommendations regarding medications, diet, and follow-up appointments.
Monitor Your Symptoms:
Keep track of your symptoms and seek medical attention if they worsen or new symptoms develop.
Maintain a Healthy Diet:
Slowly boost your fiber intake by incorporating a diverse range of fiber-rich foods into your diet. Avoid foods that may trigger symptoms, such as nuts, seeds, and popcorn, though recent studies suggest these foods may not need to be avoided.
Stay Hydrated:
Drink plenty of water throughout the day to help keep stools soft.
Stay Active:
Incorporate regular physical activity into your routine to promote overall health and digestive function.
Conclusion
Diverticulitis is a common condition that can cause significant discomfort and complications if not managed properly. By adopting a high-fiber diet, staying hydrated, exercising regularly, and following medical advice, individuals can reduce their risk of diverticulitis and manage the condition more effectively if it occurs.
If you suspect you have diverticulitis or are experiencing symptoms, consult a healthcare professional for a thorough evaluation and appropriate treatment. Remember, a proactive approach to your health is the best way to stay ahead of diverticulitis.